Ignore Bartonella and Die: Trivializing Bartonella is Like Ignoring TNT
August 1, 2007 in Science/Research by Dr. James Schaller, MD | Comments
As you read this article, Bartonella is making microscopic fat deposits in many human hearts. These will undermine the normal pace-maker stimulation in their heart and cause death. Others are weakening blood vessel walls to create a stroke. Still others with Bartonella are struggling with an agitated depression or aggressive rage that makes them prone to suicide. The psychiatric treatment of a patient with Bartonella is highly specialized and most family physicians and psychiatrists do not know how to treat a patient suffering from Bartonella-caused psychiatric disorders.
Bartonella is connected to red blood cells that are entering every human organ. Some are leaving their red blood cell carriers and entering tissues next to capillaries all over the body. They enter all organs and cause the following sample illnesses: All Psychiatric disorders, Numbness or Loss of Sensation, Dizziness,Headaches, Tremors, Irritability, Agitation, Aggression, Impulsivity, Oxygen Deprivation, Panic Attacks, Fainting, Muscle Spasms and/or Weakness, Joint Pain, Upper and Lower G.I.Tract Disorders, Kidney,Bladder, and Urogenital Disorders. Also common are: Fatigue, Sleep Disorders, Memory Problems, and Drowsiness.
Obvious physical symptoms such as Lumps in the Skin, Many types of Rashes, Polyps in or on Major Organs, Ocular Disorders, e.g., BlurredVision, Depth Perception, and Retinal Damage. This modified list from Breitschwerdt and others (Emerging Infectious Diseases June 2007; 13:pg 938ff) is a small sample of Bartonella medical ills. For example, in another series of articles, 15-25 eye ailments are listed. In the same manner, Lyme disease was initially seen as merely an arthritis disease and Babesia as a disease causing only fevers, fatigue and sweats.
We have learned with each passing year that Babesia infections have hundreds of symptoms. Bartonella is similar. It was initially seen as a virus and as having 2-3 species with American forms generally only causing a cold, a mild fever and a passing increase in lymph node size or tenderness. The reality is that thousands of articles show Bartonella harms many parts of the body and can cause multiple types of tissue injury. It is also so common that just this week, another human species was found --Bartonella rochalimae.
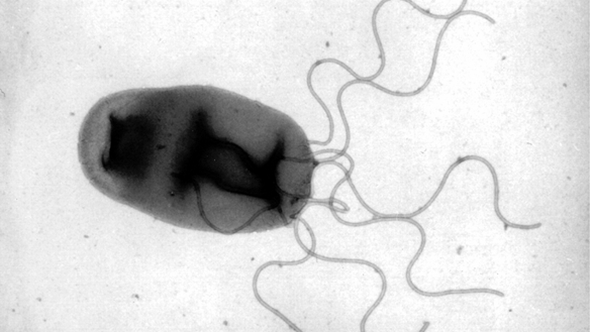
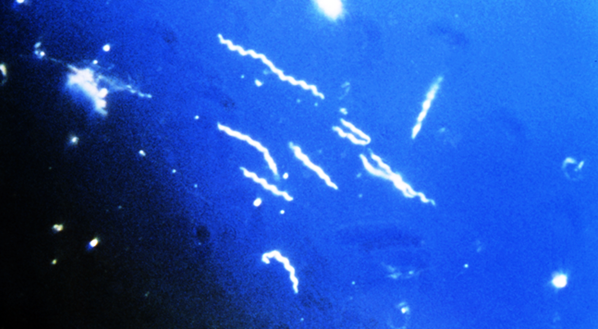
With the publication of my Babesia textbook, and the wise warnings and generous lessons of practitioners like Drs. Jemsek, Horowitz and Burrascano, I was able to consolidate their exceptional experience into a single book to help patients and physicians to quickly learn about Babesia. As you can see from the new patent pending Fry blood slides in this article,which show Babesia with many Bartonella images, you can see the discovery of a revolutionary blood smear test which shows all species of Bartonella and Babesia. The light has been turned on in the midnight kitchen, and all the largest "Bartonella bugs" can be seen crawling around in the kitchen with this special bloodstain. Currently, approximately 10 species of Bartonella and 13 species of Babesia exist which infect humans.
This specialized patent pending slide has made them markedly visible-like a July 4th firework explosion. While curing patients all over the world with this new tool to direct me, this stain also allows me to see what really kills both of these infections. I have sent the same slide to the largest labs in the USA. Not one patient has been diagnosed on a manual smear by leading large medical labs! Their stains are junk, and their ability to see these two infections are worthless. The year 2007 will mark the death of the expression "co-infection," because increasingly patients have awareness that Babesia and Bartonella are not little addendums to Lyme disease, but are often far more serious than Lyme disease. Any physician who is not well-versed in these two killing infections will not be considered competent enough to treat patients with flea and tick infections. These infections do not circle around planet "Lyme" like small moons, instead, they are their own huge planets that cause massive consequences to the human body.
Later this year I will be publishing "The Diagnosis and Treatment of Bartonella". Despite millions of books inprint, no book currently exists on the up-to-date issues of the diagnosis and treatment of Bartonella. This stunning lack of information about a profoundly common human infection has added to the danger of this infection. In Asian stories, the Ninja is felt to be a dangerous assassin because he has mastered invisibility techniques. This article is meant to be the first summary article to shine a bright lamp on the infectious Ninja - Bartonella.
Bartonella is Everywhere
Bartonella is so common that 40% of California cats have lab findings showing contact with the illness. Since 1/3 of all USA homes have a cat, this means many of the 70 million cats in the USA can playfully bite, lick or scratch a human and infect them. But one thing wrong with this 40% number is the assumption that the test used is reliable and catches every Bartonella positive cat. I have sent positive animal and human samples to many labs and they were routinely missed. So I believe DNA or PCR tests and various antibody tests (IgG/IgM) can support a diagnosis if they are positive, but remember they typically miss infected animals and humans.
In contrast to Lyme disease, Bartonella is virtually everywhere except countries near the cold northern and southern poles. The reason Bartonella is so common is that it is found in many vectors or insect carriers. Here are some sample vectors and ways a Bartonella infection can be passed.
Bartonella is carried in a number of vectors and animals, but articles that report strict limits on the location of each Bartonella species are probably in error. For example, WA-1 is a species of Babesia found in a small number of patients in Washington State. Most infectious disease physicians never tested for it, and the Sonoma health department set an extremely high bar for a positive--1:6 40, which means the Babesia is detectable after 640 dilutions. Imagine a dark blue pool diluted with clear water 640x. I wonder how often any residual blue would be seen. Once the WA-1 test was initiated, despite the absurd 1:6 40 cut off, I began to find some patients who were positive for this aggressive Babesia species on the entire East coast and throughout the southern states. In the same way, I feel when a good test begins to be used more often we will find both new human Bartonella species and current Bartonella in more regions of the world.
Bartonella and Psychiatric Symptoms
First, this emerging infection is found in cities, suburbs and rural locations. Presently routine national labs offer testing of questionable quality for only two species, but at least nine have been discovered as human infections within the last 15 years. Some authors discuss Bartonella cases having atypical presentations, with serious problems considered uncharacteristic of more routine Bartonella infections.
Some "atypical" findings include: distortion of vision, abdominal pain, severe liver and spleen tissue abnormalities, bone infection, arthritis, abscesses, skin sores, heart tissue and heart valve problems. While some articles discuss Bartonella as a cause of neurological illnesses, psychiatric illnesses have received virtually no attention. This is amazing, because almost all of my Bartonella patients have some character, mood or cognitive alterations. Further, their dosing of psychiatric medications is radically different. Some can only tolerate 1/4th of the smallest Lexapro and others need 60mgs.
The presence of Bartonella-induced psychiatric symptoms should not be surprising for a number of reasons. First, psychiatric disorders are brain disorders and Bartonella is documented as causing many diverse neurological brain disorders. Bartonella infections are associated with red blood cells (RBC), which allow small Bartonella bacteria, a fraction of the RBC cell size to enter the brain's vascular system. These Bartonella-infected cells penetrate brain tissue. Finally,with 9-10 species or subspecies that can infect humans, it is possible this larger number of species can produce a wider range of signs and symptoms - some of which might be psychiatric in nature. Below, I offer a medical case with psychiatric symptoms that emerged during a Bartonella infection.
A Sample Case
A 41 year-old male minister from Wisconsin was reported by his wife, best friends and children to have a personality change after a camping trip in North Carolina. After the trip, the patient described a small right-sided "aching" armpit lymph node and as having a "slight fever feeling." He reported removing three Ixodes deer ticks that resembled "large dust particles glued to his leg and shoulder."
Five weeks later, he reported an "enlarged and very annoying" right-sided armpit lymph node, feelings of excessive warmth, irritability, severe insomnia and new-onset eccentric rage. He also reported a new sensitivity to otherwise only slightly annoying smells and sounds. His afternoon temperatures were 98.7-99.9 °F, which he recorded every 3 days on the advice of a relative who was a Physician Assistant.
His internist found the patient to be negative for Lyme disease using the CDC two-tier surveillance testing procedure performed at Quest diagnostics and IGeneX's PCR and Western Blot test. It was felt that the patient might have Bartonella based on his unilateral lymph node symptom and Ixodes attachment. This physician felt that since the duration of the lymph node ache was at least five weeks, that "atypical" Bartonella should be considered in the differential. "Atypical"means that the man had more than a simple cold, passing sore throat and transient low-grade fever. The patient was ordered a Bartonella henselae IgG and IgM along with other lab testing which was negative, including a PCR test for Bartonella. However, the Fry Blood Smear Test came back as positive.
During the next two weeks, the patient developed serious agitation, panic attacks and major depression. He was so restless that he threw objects such as kitchen glasses, a baseball, and a chair into his home's drywall, leaving significant indentations. He was previously unknown to use insults or to curse at people, and now he did both almost daily, particularly to his spouse. Minor interpersonal infractions that would not usually produce a comment from the patient now resulted in screaming and the use of obscenities, yet he slept 8-9 hours per day and had normal speech speed and enunciation patterns.
He was referred to an adult psychiatrist and diagnosed with Bipolar disorder, despite having no genetic history or any previous history of depression or mania. The patient gained 15 pounds in weeks on 1250 mg per day of valproic acid (Depakote), and requested another treatment. He was then prescribed lithium carbonate, 300 mg at breakfast, lunch and dinner, with 600 mg once in the evening (blood level 1.1mEq/L). These medications had no clear clinical effect on the patient's agitation, mood extremes or severe boredom with hopelessness. They were stopped after at least three-week trials. It was unclear to the patient, his family, and his psychiatrist whether either medication offered more than a slight benefit to limiting his reactivity and eccentric anger.
A trial of quetiapine (Seroquel) at 12.5 mg in the morning, afternoon and 50 mg at bedtime helped significantly for 3 weeks, but then it stopped controlling his agitation and other dysfunctional behaviors. So he was tried on a higher dose of 25 mg in the morning, 25 mg in the afternoon and 100 mg at bed. The patient surprisingly reported that he felt "good" and "content" on this antipsychotic medication. At this point, the patient was diagnosed with Bartonella and treated with azithromycin 500 mg (Zithromax) at dinner and rifabutin 300 mg (Mycobutin) per day. Duringthe first 2 weeks of treatment on these medications, the patient's anxiety increased and he experienced five panic attacks. He was highly reactive, emotionally volatile and markedly irritable. His quetiapine was increased to 50 mg at breakfast and lunch, and 200 mg once in the evening, with good control of his increased psychiatric morbidity.
After five weeks on this dual-antibiotic treatment, the patient began to exhibit sleepiness. His quetiapine dose was reduced to 25 mg at breakfast and 75 mg at bedtime, with no return of agitation or mood lability. The internist's reading left him uncertain of the ideal dose of antibiotics and duration of treatment for this suspected Bartonella infection. But when the patient's lymph node complaints ended abruptly in 48 hours, following 8 weeks of antibiotics, the medications were stopped. The patient has significantly improved in his psychiatric symptoms and he now remains only on escitalopram (Celexa) 5 mg and quetiapine 12.5 mg in the morning, and 37.5 mg once in the evening. His baseline personality is felt to be 90% according to his spouse and closest friend.
We suggest this man's psychiatric problems support a Bartonella presentation. Our reasons are due to the sudden appearance of these symptoms following clear Ixodes attachments, the presence of an acute, unilateral and uncomfortable armpit lymph node, a "slight fever" feeling, a low-positive Bartonella serology result, and a positive response to two antibiotics which are felt to be effective against Bartonella.
Further, his emotional improvement occurred nearly simultaneous to his enlarged lymph node normalization.
This pastor wants his story told because he feels he "lost himself" and he now believes that many people who do reckless things like start fights, drink or do drugs impulsively, abuse family and friends, do impulsive sexual acts, drive with "road rage" and do other angry, impulsive, reactive behavior may be behaving this way due to a brain Bartonella infection. He does not know how many but as he meets more and more individuals with these troubles he reports discerning a medical fog.
"I cannot explain it, but I can just feel someone has what I had, but unfortunately, most do not listen to me and consider testing."
I have tested a few of those he diagnosed and they all had at least two tick or flea infections with labs that showed systemic abnormal inflammation. The pastor feels "blessed" that he had an abnormal lymph node to help with diagnosis since he has personally found patients with Bartonella and most had no lymph node abnormalities and no rashes.
Treatment
Since there is much debate about optimal treatment, and because I am involved in a number of treatment studies using a wide range of treatments for Bartonella, I will not address Bartonella treatment in this article. I will however mention that this is a complex area. Medications felt to work may only work with some Bartonella from certain regions, and that dosing often has to be higher then normal. Further, we generally find better results with multiple treatments at the same time. Finally, it is a fact that Bartonella, like many other Gram-negative bacteria, have external biotoxins. However, in contrast to most biotoxins from bacteria, Bartonella biotoxins seem to turn off the immune system and the inflammation system in some parts, which allows it to hide even with large numbers in the bloodstream. Bartonella also appears to occasionally be able to make biofilms to protect itself from antibiotics.
Bartonella is connected to red blood cells that are entering every human organ. Some are leaving their red blood cell carriers and entering tissues next to capillaries all over the body. They enter all organs and cause the following sample illnesses: All Psychiatric disorders, Numbness or Loss of Sensation, Dizziness,Headaches, Tremors, Irritability, Agitation, Aggression, Impulsivity, Oxygen Deprivation, Panic Attacks, Fainting, Muscle Spasms and/or Weakness, Joint Pain, Upper and Lower G.I.Tract Disorders, Kidney,Bladder, and Urogenital Disorders. Also common are: Fatigue, Sleep Disorders, Memory Problems, and Drowsiness.
Obvious physical symptoms such as Lumps in the Skin, Many types of Rashes, Polyps in or on Major Organs, Ocular Disorders, e.g., BlurredVision, Depth Perception, and Retinal Damage. This modified list from Breitschwerdt and others (Emerging Infectious Diseases June 2007; 13:pg 938ff) is a small sample of Bartonella medical ills. For example, in another series of articles, 15-25 eye ailments are listed. In the same manner, Lyme disease was initially seen as merely an arthritis disease and Babesia as a disease causing only fevers, fatigue and sweats.
We have learned with each passing year that Babesia infections have hundreds of symptoms. Bartonella is similar. It was initially seen as a virus and as having 2-3 species with American forms generally only causing a cold, a mild fever and a passing increase in lymph node size or tenderness. The reality is that thousands of articles show Bartonella harms many parts of the body and can cause multiple types of tissue injury. It is also so common that just this week, another human species was found --Bartonella rochalimae.
With the publication of my Babesia textbook, and the wise warnings and generous lessons of practitioners like Drs. Jemsek, Horowitz and Burrascano, I was able to consolidate their exceptional experience into a single book to help patients and physicians to quickly learn about Babesia. As you can see from the new patent pending Fry blood slides in this article,which show Babesia with many Bartonella images, you can see the discovery of a revolutionary blood smear test which shows all species of Bartonella and Babesia. The light has been turned on in the midnight kitchen, and all the largest "Bartonella bugs" can be seen crawling around in the kitchen with this special bloodstain. Currently, approximately 10 species of Bartonella and 13 species of Babesia exist which infect humans.
This specialized patent pending slide has made them markedly visible-like a July 4th firework explosion. While curing patients all over the world with this new tool to direct me, this stain also allows me to see what really kills both of these infections. I have sent the same slide to the largest labs in the USA. Not one patient has been diagnosed on a manual smear by leading large medical labs! Their stains are junk, and their ability to see these two infections are worthless. The year 2007 will mark the death of the expression "co-infection," because increasingly patients have awareness that Babesia and Bartonella are not little addendums to Lyme disease, but are often far more serious than Lyme disease. Any physician who is not well-versed in these two killing infections will not be considered competent enough to treat patients with flea and tick infections. These infections do not circle around planet "Lyme" like small moons, instead, they are their own huge planets that cause massive consequences to the human body.
Later this year I will be publishing "The Diagnosis and Treatment of Bartonella". Despite millions of books inprint, no book currently exists on the up-to-date issues of the diagnosis and treatment of Bartonella. This stunning lack of information about a profoundly common human infection has added to the danger of this infection. In Asian stories, the Ninja is felt to be a dangerous assassin because he has mastered invisibility techniques. This article is meant to be the first summary article to shine a bright lamp on the infectious Ninja - Bartonella.
Bartonella is Everywhere
Bartonella is so common that 40% of California cats have lab findings showing contact with the illness. Since 1/3 of all USA homes have a cat, this means many of the 70 million cats in the USA can playfully bite, lick or scratch a human and infect them. But one thing wrong with this 40% number is the assumption that the test used is reliable and catches every Bartonella positive cat. I have sent positive animal and human samples to many labs and they were routinely missed. So I believe DNA or PCR tests and various antibody tests (IgG/IgM) can support a diagnosis if they are positive, but remember they typically miss infected animals and humans.
In contrast to Lyme disease, Bartonella is virtually everywhere except countries near the cold northern and southern poles. The reason Bartonella is so common is that it is found in many vectors or insect carriers. Here are some sample vectors and ways a Bartonella infection can be passed.
- Four Bartonella species have been found in dust mites.
- Flea bites.
- Flea feces - Bartonella live at least nine days in this substance. If it touches a human mouth, nose, or eye, Bartonella can infect a person.
- Cats and dogs can carry this infection in their paws and saliva, and scratch, lick or bite you.
- Lice - such as forms found in schools or dirty areas
- Ticks - in some tick research areas, in which Lyme disease exists in high concentrations, surprisingly, Bartonella is sometimes even more common than Lyme disease.
- Flies - some carry this infection and pass it on to mammals. I suspect as laboratory science improves, we will find this infection in more flies in coming years
- Birth infection - examination of fetal pregnancy tissue shows that Bartonella clearly infects the placenta, and infected baby mice are born smaller; further, Bartonella decreases successful pregnancies.
Bartonella is carried in a number of vectors and animals, but articles that report strict limits on the location of each Bartonella species are probably in error. For example, WA-1 is a species of Babesia found in a small number of patients in Washington State. Most infectious disease physicians never tested for it, and the Sonoma health department set an extremely high bar for a positive--1:6 40, which means the Babesia is detectable after 640 dilutions. Imagine a dark blue pool diluted with clear water 640x. I wonder how often any residual blue would be seen. Once the WA-1 test was initiated, despite the absurd 1:6 40 cut off, I began to find some patients who were positive for this aggressive Babesia species on the entire East coast and throughout the southern states. In the same way, I feel when a good test begins to be used more often we will find both new human Bartonella species and current Bartonella in more regions of the world.
Bartonella and Psychiatric Symptoms
First, this emerging infection is found in cities, suburbs and rural locations. Presently routine national labs offer testing of questionable quality for only two species, but at least nine have been discovered as human infections within the last 15 years. Some authors discuss Bartonella cases having atypical presentations, with serious problems considered uncharacteristic of more routine Bartonella infections.
Some "atypical" findings include: distortion of vision, abdominal pain, severe liver and spleen tissue abnormalities, bone infection, arthritis, abscesses, skin sores, heart tissue and heart valve problems. While some articles discuss Bartonella as a cause of neurological illnesses, psychiatric illnesses have received virtually no attention. This is amazing, because almost all of my Bartonella patients have some character, mood or cognitive alterations. Further, their dosing of psychiatric medications is radically different. Some can only tolerate 1/4th of the smallest Lexapro and others need 60mgs.
The presence of Bartonella-induced psychiatric symptoms should not be surprising for a number of reasons. First, psychiatric disorders are brain disorders and Bartonella is documented as causing many diverse neurological brain disorders. Bartonella infections are associated with red blood cells (RBC), which allow small Bartonella bacteria, a fraction of the RBC cell size to enter the brain's vascular system. These Bartonella-infected cells penetrate brain tissue. Finally,with 9-10 species or subspecies that can infect humans, it is possible this larger number of species can produce a wider range of signs and symptoms - some of which might be psychiatric in nature. Below, I offer a medical case with psychiatric symptoms that emerged during a Bartonella infection.
A Sample Case
A 41 year-old male minister from Wisconsin was reported by his wife, best friends and children to have a personality change after a camping trip in North Carolina. After the trip, the patient described a small right-sided "aching" armpit lymph node and as having a "slight fever feeling." He reported removing three Ixodes deer ticks that resembled "large dust particles glued to his leg and shoulder."
Five weeks later, he reported an "enlarged and very annoying" right-sided armpit lymph node, feelings of excessive warmth, irritability, severe insomnia and new-onset eccentric rage. He also reported a new sensitivity to otherwise only slightly annoying smells and sounds. His afternoon temperatures were 98.7-99.9 °F, which he recorded every 3 days on the advice of a relative who was a Physician Assistant.
His internist found the patient to be negative for Lyme disease using the CDC two-tier surveillance testing procedure performed at Quest diagnostics and IGeneX's PCR and Western Blot test. It was felt that the patient might have Bartonella based on his unilateral lymph node symptom and Ixodes attachment. This physician felt that since the duration of the lymph node ache was at least five weeks, that "atypical" Bartonella should be considered in the differential. "Atypical"means that the man had more than a simple cold, passing sore throat and transient low-grade fever. The patient was ordered a Bartonella henselae IgG and IgM along with other lab testing which was negative, including a PCR test for Bartonella. However, the Fry Blood Smear Test came back as positive.
During the next two weeks, the patient developed serious agitation, panic attacks and major depression. He was so restless that he threw objects such as kitchen glasses, a baseball, and a chair into his home's drywall, leaving significant indentations. He was previously unknown to use insults or to curse at people, and now he did both almost daily, particularly to his spouse. Minor interpersonal infractions that would not usually produce a comment from the patient now resulted in screaming and the use of obscenities, yet he slept 8-9 hours per day and had normal speech speed and enunciation patterns.
He was referred to an adult psychiatrist and diagnosed with Bipolar disorder, despite having no genetic history or any previous history of depression or mania. The patient gained 15 pounds in weeks on 1250 mg per day of valproic acid (Depakote), and requested another treatment. He was then prescribed lithium carbonate, 300 mg at breakfast, lunch and dinner, with 600 mg once in the evening (blood level 1.1mEq/L). These medications had no clear clinical effect on the patient's agitation, mood extremes or severe boredom with hopelessness. They were stopped after at least three-week trials. It was unclear to the patient, his family, and his psychiatrist whether either medication offered more than a slight benefit to limiting his reactivity and eccentric anger.
A trial of quetiapine (Seroquel) at 12.5 mg in the morning, afternoon and 50 mg at bedtime helped significantly for 3 weeks, but then it stopped controlling his agitation and other dysfunctional behaviors. So he was tried on a higher dose of 25 mg in the morning, 25 mg in the afternoon and 100 mg at bed. The patient surprisingly reported that he felt "good" and "content" on this antipsychotic medication. At this point, the patient was diagnosed with Bartonella and treated with azithromycin 500 mg (Zithromax) at dinner and rifabutin 300 mg (Mycobutin) per day. Duringthe first 2 weeks of treatment on these medications, the patient's anxiety increased and he experienced five panic attacks. He was highly reactive, emotionally volatile and markedly irritable. His quetiapine was increased to 50 mg at breakfast and lunch, and 200 mg once in the evening, with good control of his increased psychiatric morbidity.
After five weeks on this dual-antibiotic treatment, the patient began to exhibit sleepiness. His quetiapine dose was reduced to 25 mg at breakfast and 75 mg at bedtime, with no return of agitation or mood lability. The internist's reading left him uncertain of the ideal dose of antibiotics and duration of treatment for this suspected Bartonella infection. But when the patient's lymph node complaints ended abruptly in 48 hours, following 8 weeks of antibiotics, the medications were stopped. The patient has significantly improved in his psychiatric symptoms and he now remains only on escitalopram (Celexa) 5 mg and quetiapine 12.5 mg in the morning, and 37.5 mg once in the evening. His baseline personality is felt to be 90% according to his spouse and closest friend.
We suggest this man's psychiatric problems support a Bartonella presentation. Our reasons are due to the sudden appearance of these symptoms following clear Ixodes attachments, the presence of an acute, unilateral and uncomfortable armpit lymph node, a "slight fever" feeling, a low-positive Bartonella serology result, and a positive response to two antibiotics which are felt to be effective against Bartonella.
Further, his emotional improvement occurred nearly simultaneous to his enlarged lymph node normalization.
This pastor wants his story told because he feels he "lost himself" and he now believes that many people who do reckless things like start fights, drink or do drugs impulsively, abuse family and friends, do impulsive sexual acts, drive with "road rage" and do other angry, impulsive, reactive behavior may be behaving this way due to a brain Bartonella infection. He does not know how many but as he meets more and more individuals with these troubles he reports discerning a medical fog.
"I cannot explain it, but I can just feel someone has what I had, but unfortunately, most do not listen to me and consider testing."
I have tested a few of those he diagnosed and they all had at least two tick or flea infections with labs that showed systemic abnormal inflammation. The pastor feels "blessed" that he had an abnormal lymph node to help with diagnosis since he has personally found patients with Bartonella and most had no lymph node abnormalities and no rashes.
Treatment
Since there is much debate about optimal treatment, and because I am involved in a number of treatment studies using a wide range of treatments for Bartonella, I will not address Bartonella treatment in this article. I will however mention that this is a complex area. Medications felt to work may only work with some Bartonella from certain regions, and that dosing often has to be higher then normal. Further, we generally find better results with multiple treatments at the same time. Finally, it is a fact that Bartonella, like many other Gram-negative bacteria, have external biotoxins. However, in contrast to most biotoxins from bacteria, Bartonella biotoxins seem to turn off the immune system and the inflammation system in some parts, which allows it to hide even with large numbers in the bloodstream. Bartonella also appears to occasionally be able to make biofilms to protect itself from antibiotics.
About the author
Dr. James Schaller, MD has done some of the most extensive research regarding Bartonella world wide.
Dr. Schaller is the author of 20 books including: The Diagnosis and Treatment of Babesia, Mold Illness and Mold Remediation Made Simple, The Complete Guide to Artemisinin, When Traditional Medicine Fails, 100 Solutions to Out of Control Youth, Suboxone-Pain Treatment with Addiction Relief.
Dr. Schaller is a strong advocate for looking at many treatments and illness causes as can be seen from his main website: PersonalConsult.com.
Dr. Schaller is the author of 20 books including: The Diagnosis and Treatment of Babesia, Mold Illness and Mold Remediation Made Simple, The Complete Guide to Artemisinin, When Traditional Medicine Fails, 100 Solutions to Out of Control Youth, Suboxone-Pain Treatment with Addiction Relief.
Dr. Schaller is a strong advocate for looking at many treatments and illness causes as can be seen from his main website: PersonalConsult.com.
latest posts
tags
Disclaimer: The information on this website is not a substitute for professional medical advice.
Always consult with your treating physician before altering any treatment protocol.
Always consult with your treating physician before altering any treatment protocol.